I Took Control of my Biological Clock at Age 30
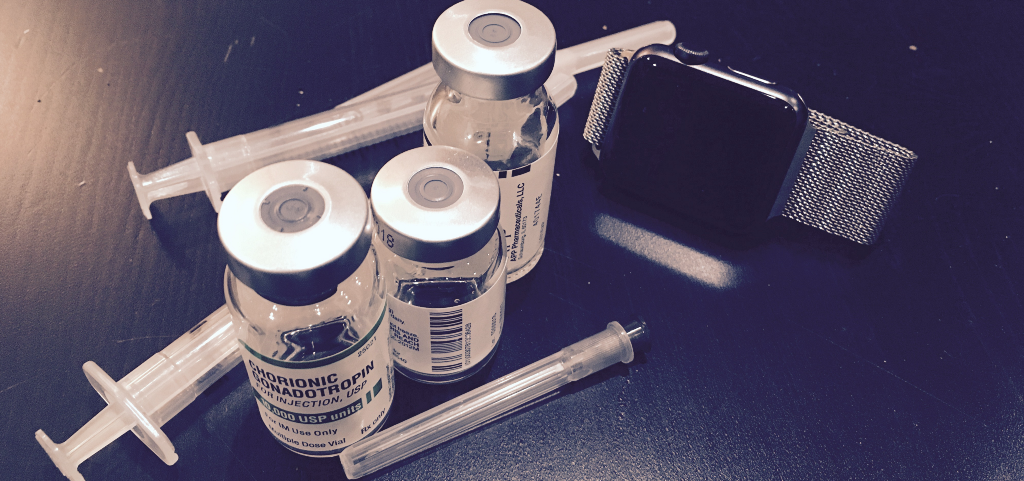
My San Francisco apartment is generally stacked with liquor, laptops and leftovers from last weeks’ dinner party. But for now, it has been transformed into a nursing station, stacked high with cartons of prescription drugs, syringes, gauze, alcohol wipes, even a sharps container.
I barely take Tylenol for headaches or Midol for period cramps. But for the past 11 days I’ve been injecting myself daily with with heavy doses of gonadal-stimulating hormones. In a few hours, I’ll check myself in for an outpatient surgery where a doctor will extract roughly 5–15 of my eggs by sticking a long needle through my vaginal wall in to each of my ovaries. The whole process will cost about as much as a lightly-used 2014 Honda Civic.
Merry Christmas, me.
Egg freezing (formally, “Cryopreservation”) is a physically, mentally and emotionally disruptive process: injections, mood swings, body changes. So why is 30-year-old, healthy, seemingly normal woman with 10 fingers, 10 toes, and a full pipeline on every dating app, freezing her eggs?
I’m an economist so maybe I’m drawn to this way of thinking, but I don’t think it takes a quant to understand what it means to be almost 31, female, and single. A simple Google search returns the well-known commentary around female fertility and egg health/genetic degradation starting after age 35. Many doctors quoted online seem to recommend a first pregnancy by about age 34, especially for women intending on having more than one child.
So, using my best life-algebra, I calculate:
Age 34, (-) minus 2 years to be married to someone before kids, (-) minus 1.5 years to meet, date and marry someone = 30.5.
Since I’m almost 31, having not found Mr or Ms. Right by last month means I’m on a path to compromising the potential health of my future children, unless a take a significant short cut in my future partner evaluation timeline. Not exactly what I want in my latest Tinder tagline.

Its *not* just about partner selection
For many women, regardless of whether we definitely want biological children someday, after about age 29, there settles in this pressure of ‘fertility fog’ over a wide range of life decisions. Not only does competence as a potential parent begin to weigh more heavily in partner selection, but other critical decisions like job selection, budgeting & financial planning, social ties — all begin to take potential childbearing and maternity more seriously into consideration. For those ready to take this step — great. But for many women, feeling like you’re ‘on the clock’ can result in the pressure to compromise on the qualities you accept in a partner and reduce risk tolerance at work.
For many women, feeling like you’re ‘on the clock’ can result in the pressure to compromise on the qualities you accept in a partner and reduce risk tolerance at work.
Altogether, I was feeling out of control of my own body — as if my decisions needed to be increasingly driven by my fertility calculus, not by the many factors I want to and historically have considered in big life decisions (i.e. impact, size and scale of the challenge, intellectual engagement, etc). The daughter of a low-income, single mother from a small town in Canada, I worked hard to have the freedoms I experience today in my work and lifestyle choices. I wanted control of my body and reproductive timeline back. So, I reached out to my primary care doctor and asked for a referral.
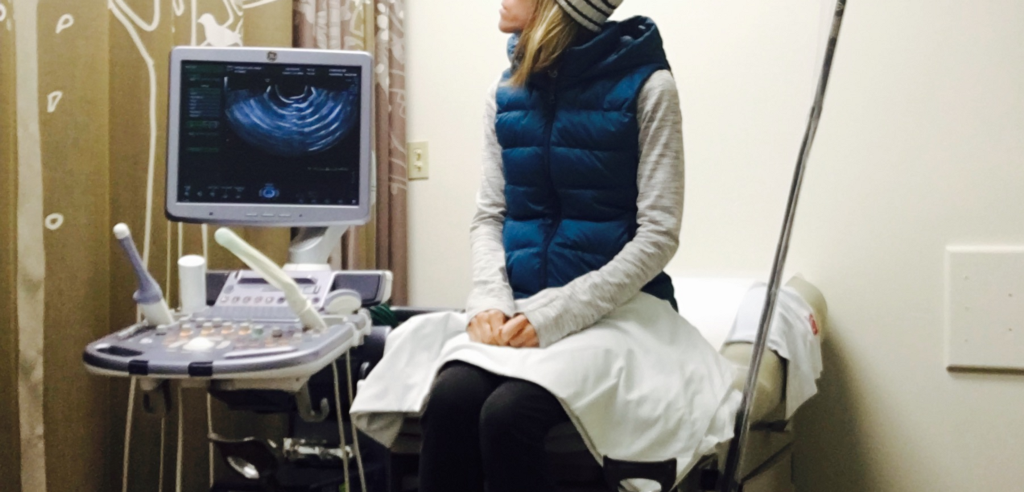
The process is intimidating
I would be a really bad drug addict, or so I discovered.
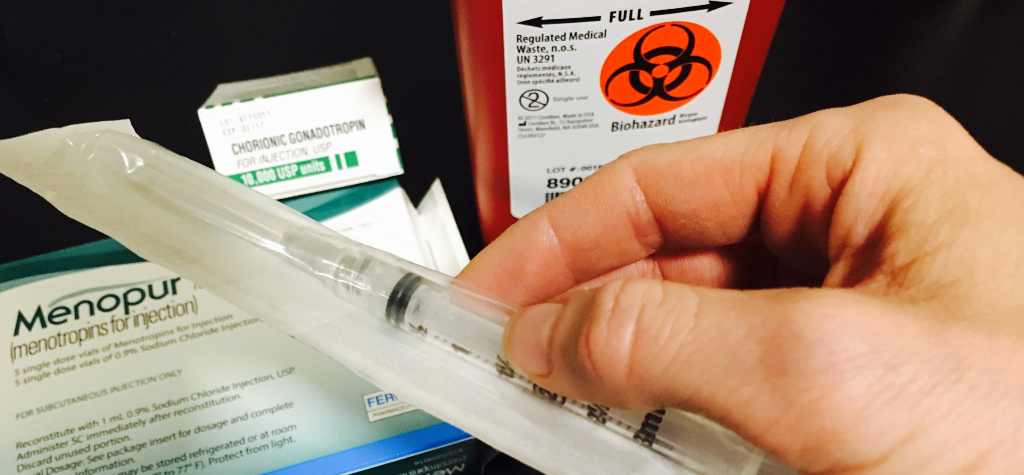
To get a female body to cultivate 10–20x the normal eggs in one monthly cycle, a high-dosage, 11-day regimen of (egg) “follicle-stimulating” hormones is required to turbo-charge the normal monthly process. These are the types of hormones generally found in a woman’s body, but at much lower natural levels. The hormones can only be received through sub-cutaneous injection, and since they are taken daily for 11 days, the woman is required to self-administer the injections at home.
I’m not a wimp (I played college and high school rugby, ran a marathon, have a tattoo, etc) — but I definitely panicked during the training on self-administered hormone shots. I had figured that since normal people needed to self-inject very specific quantities of medicine to not screw the process up, there would be some method or device that helped us self-inject — that somehow made it easier —like a special clamp or ‘Smart Needle’: one click and a little prick and you’re done. Well, no such luck. I needed to use real, basic needles to inject 1-2ml of liquid hormone slowly into my body in two shots — daily — for 10+ days. At work, I’m known for my strong crisis-situation management skills. But in the tiny consultation room that day, I felt overwhelmed.
Thank goodness I caught wind of a start-up business by some nurses who can come to your home and professionally administer the shots. “IVF Concierge” — look them up if you are considering the process! They are *fantastic.* While the service is expensive, its worth it to have a professional get it right on the first shot (pun intended?).
Intimidating or not, women want it anyway
Almost every woman I’ve spoken to since I decided to freeze my eggs says she would want to do it too but can’t afford the ~$12,000 for a cryopreservation cycle, from my hair stylist (who lovingly streaked my hair pink when asked to on day 3 of my hormone therapy), to many of my close female friends who are mostly professionals in finance, technology, law, medicine and academia.
…it is not only the highly career-focused women, but those from all walks of life who seem to want this option.
It’s not only the highly career-focused women, but those from all walks of life who seem to want this option. Even if you presume only a quarter or half of those women would actually go through with the process, that’s still a large number when scaled across the whole eligible population. Married & unmarried, the women I spoke to simply wanted the same freedoms as men do: to choose to have children earlier or later in their lives without the guilt of a direct trade-off between having any / healthy children the longer they wait. Having the freedom to kick the proverbial can down the road is a freedom Nature doesn’t afford women.
Having the freedom to kick the proverbial can down the road is a freedom Nature doesn’t afford women.
Eggspensive but eggaliatrian
If I’m the right age to cryopreserve and so many people I know say they want it, why am I the only woman I know with a box full of drugs in her living room?
Realistically, the biggest difference for me in this calculus versus other women my age is that my employment-based health insurance covers the >$10K cost of the procedure and medications.
Currently, only a handful of employers seem to see the value in providing cryopreservation coverage, and the majority of others either don’t, or have yet to realistically consider it. In my view, providing cryopreservation coverage not only increases an employers’ competitiveness in the marketplace for female employees, but also is a great way for companies to put their ‘money where their mouth is’ on the topic of gender equality efforts in the workplace.
Cryopreservation health insurance coverage is a great way for companies to put their ‘money where their mouth is’ on the topic of gender equality efforts in the work place.
By giving women greater flexility in when they incur the tough demands of pregnancy & post-natal child care, companies can help create a more equal experience between men and women workers.
A bit more choice for women around pregnancy and family timing could go a long way on several lingering workplace gender equality issues, like the number of women in executive positions and on boards, and the gender pay gap. A 2015 White House Council of Economic Advisors brief on the Gender Pay Gap noted that:
“…motherhood is associated with a wage penalty and lower wage gains later in a woman’s career,” and that “Research has shown that delaying child birth for one year can increase a woman’s total career earnings and experience by 9 percent.”
These statistics really resonate with my experience — I’ve lost track of how many times I’ve heard my female friends express the pressure that right now “every year counts,” for their financial trajectory and promotions.
Overall, I’m deeply thankful that my employer has provided this option for me, and am hopeful that over time the benefit will become a standard. And I hope that by sharing my experience with the bad and honestly not-so-bad parts of the egg freezing journey, I can de-mystify the experience for women who are considering the option. Please feel free to reach out to me if you want to hear from someone who’s been through the process, or even if you just want someone to listen to your fears and concerns. It’s daunting, and it isn’t comfortable, but it is an option for regaining some basic control over reproductive timing. Good luck!
Special thanks to Saul Carlin, Alexander Campbell, Jake Wachman and Joyce Zhang for your feedback.
Support The Billfold
The Billfold continues to exist thanks to support from our readers. Help us continue to do our work by making a monthly pledge on Patreon or a one-time-only contribution through PayPal.
Comments